A Guide to HIPAA-Compliant Medical Equipment Disposal Services Nationwide and Local

When your healthcare facility—whether it's a local clinic in Atlanta or a hospital system with locations across the country—gets rid of old equipment, it’s not just a matter of making space. It's a critical security task. True HIPAA-compliant medical equipment disposal services are about making sure the sensitive patient data on those devices is gone for good, protecting your organization from staggering fines and a damaged reputation, no matter where you are located.
Why Compliant Disposal Isn’t Just an Option—It’s a Mandate
Getting rid of medical equipment isn’t as simple as unplugging a machine and rolling it out to the loading dock. Today’s medical devices—from complex MRI machines and lab analyzers to what seem like simple patient monitors—are packed with data storage. They often hold huge amounts of electronic Protected Health Information (ePHI), creating a massive liability if they aren't disposed of correctly, both for local providers and nationwide health networks.
Think of it this way: you would never leave unlocked patient filing cabinets in a public alley. Improperly disposing of an old server, an ultrasound machine, or even an office printer from a clinical area is the digital version of that exact mistake. These devices can hold onto names, diagnoses, medical record numbers, and other private data long after they’ve been taken out of service.

The Staggering Risks of Getting It Wrong
The consequences of a slip-up are severe and go far beyond a simple slap on the wrist. For any healthcare organization, from a single clinic in Phoenix to a national hospital network, a single data breach can set off a chain reaction of terrible outcomes.
The risks include:
- Massive Financial Penalties: HIPAA fines aren't small change; they can reach millions of dollars for a single violation. In 2023, one health system was hit with $49 million in penalties after PHI was found in unsecured trash bins—a powerful reminder of the financial stakes.
- Irreversible Reputational Damage: Patient trust is everything in healthcare. A data breach shatters that trust, causing patients to go elsewhere and destroying a reputation that took years to build.
- Legal and Operational Headaches: Cleaning up after a breach means expensive forensic investigations, patient notifications, and the threat of class-action lawsuits, all of which pull critical resources away from patient care.
A data breach is not just an IT problem; it's a business catastrophe. The average cost of a healthcare data breach has soared to $10.93 million, highlighting the immense financial threat posed by improperly retired assets.
The Law Is Clear: Data Must Be Destroyed
Federal law doesn't leave any room for interpretation here. Rules under HIPAA, like 45 CFR 164.530(c), require that covered entities make PHI "completely unreadable and unrecoverable" before disposal. This isn't a suggestion; it's a rule that is especially critical for equipment that stores ePHI, such as MRI machines, patient monitors, and EHR servers.
It's easy to forget just how many devices in a healthcare setting store sensitive data. Here’s a quick look at some common equipment and the risks they pose.
Quick Guide to ePHI Risks in Common Medical Equipment
| Equipment Type | Potential ePHI Stored | Primary Disposal Risk |
|---|---|---|
| Diagnostic Imaging | Patient names, scans, demographics | Data can be recovered from internal hard drives if not properly wiped or destroyed. |
| Patient Monitors | Vitals, patient IDs, treatment history | Onboard memory can retain a stream of patient data that remains accessible. |
| Lab Analyzers | Test results, patient identifiers | Internal computers or connected storage can hold thousands of patient records. |
| EHR/EMR Servers | Complete patient medical records | The "gold mine" of PHI. Drives must be physically destroyed or wiped to DoD standards. |
| Medical Carts/Workstations | Login credentials, cached patient data | Often have integrated computers with hard drives that store information locally. |
| Office Equipment | Scanned documents, faxes, print logs | Printers, scanners, and copiers have hard drives that can store images of every document. |
As you can see, the risk is everywhere. With regulators looking closer at chain-of-custody gaps—and with 67% of HIPAA breaches originating from IT incidents—working with a certified disposal partner has become non-negotiable.
For any organization, from a small university lab in Houston to a large hospital system serving multiple states, using professional HIPAA-compliant disposal services is an essential safeguard. Securely managing the end-of-life for these assets is just as important as protecting data on your active network. In fact, many organizations find that a comprehensive IT asset disposal strategy is the best way to manage these risks from start to finish.
Decoding Your HIPAA Obligations for Equipment Disposal
When you're retiring old medical equipment, figuring out your responsibilities under the Health Insurance Portability and Accountability Act (HIPAA) is absolutely critical. These aren't just guidelines; they're strict legal rules designed to keep sensitive patient information safe. Getting it right means understanding both the HIPAA Privacy Rule and the Security Rule.
The Privacy Rule covers the big picture of protecting patient records. But the Security Rule is what really matters here—it deals specifically with electronic Protected Health Information (ePHI). That’s all the data hiding on the hard drives and memory chips inside your MRI machines, patient monitors, servers, and even your office copiers.
Your Responsibility Doesn’t End at the Loading Dock
One of the most common—and dangerous—mistakes is thinking your responsibility for patient data ends the second a piece of equipment is wheeled out of your facility. That’s just not true. Your legal duty follows that data wherever it goes.
Think of it this way: you wouldn't just drop a patient off at another hospital's front door. You’d make sure there was a secure, documented handoff to another qualified professional. Disposing of equipment with ePHI on it demands that same level of care.
Your duty of care continues until that data is confirmed to be permanently and verifiably destroyed. Simply handing a device over to a recycler or scrap dealer without this confirmation is a direct path to a HIPAA violation.
This is why a formal partnership is so important. As healthcare organizations work through equipment disposal, understanding the wider context of the Significance Of Privacy Rights And Corporate Responsibilities is key to staying compliant and keeping patient trust.
The Business Associate Agreement: A Critical First Step
When you hire any outside vendor to handle ePHI, including a company providing HIPAA-compliant medical equipment disposal services on a local or national scale, they legally become what's known as a "Business Associate." Before they lay a hand on a single hard drive, you must have a signed Business Associate Agreement (BAA) in place.
A BAA is a formal contract that does a few very important things:
- Defines Responsibilities: It spells out exactly what the vendor must do to protect the ePHI you've entrusted to them.
- Establishes Liability: The agreement makes the vendor directly liable for any data breaches that happen on their end, sharing the legal and financial risk.
- Requires Compliance: It legally binds your disposal partner to follow all the relevant rules of the HIPAA Security Rule.
Without a BAA, your organization is on the hook for all liability, even if the breach was entirely your vendor’s fault. It is the single most important document for creating a compliant partnership. This is a non-negotiable step for any facility, and it sets the foundation for a secure process that includes responsible handling as part of a medical equipment recycling program.
Your Proof of Compliance: The Certificate of Destruction
Right after the BAA, the next critical piece of paper you need is the Certificate of Destruction. This document is your official, auditable proof that you did your part and met your HIPAA obligations. It’s the final link in the chain, confirming that your ePHI was made completely unrecoverable.
A legitimate Certificate of Destruction will always include these key details:
- A unique serial number for tracking and auditing.
- A detailed list of the items destroyed, ideally with their individual serial numbers.
- The specific method of destruction used (e.g., shredding, multi-pass wiping).
- The date and location where the destruction occurred.
- An official signature from the vendor who did the work.
If you ever face a HIPAA audit, this certificate is your best friend. It proves you not only hired a qualified partner but also got confirmation that the job was done to legal standards, closing the loop on your compliance duties.
Choosing the Right Data Destruction Method for Your Assets
Once you’ve got a handle on your legal obligations for equipment disposal, it’s time to move from theory to practice. The reality is, not all data storage is the same, and not every piece of equipment has the same final destination. This means a one-size-fits-all approach to data destruction isn't just clumsy—it’s a recipe for non-compliance.
Deciding how to make electronic Protected Health Information (ePHI) completely unrecoverable is a huge responsibility. It’s all about matching the right destruction method to the asset, how it stores data, and what your organization plans to do with the equipment next. A professional HIPAA-compliant medical equipment disposal service, whether operating locally or nationwide, lives and breathes this process, guiding you to the most secure and practical solution for every single device.
Comparing Data Destruction Methods for HIPAA Compliance
To meet HIPAA's standard of rendering data "unreadable and unrecoverable," the National Institute of Standards and Technology (NIST) gives us a framework with three main methods. Each one offers a different level of security, like the difference between a simple deadbolt, a bank vault door, and welding the door shut for good.
Here's a quick breakdown of how they stack up:
| Method | Description | Best For | HIPAA Compliance Level |
|---|---|---|---|
| Clearing (Wiping) | Software overwrites existing data with random 1s and 0s, often in multiple passes. | Reusable assets like PCs, laptops, and servers that will be resold or redeployed. | Good: Secure when a multi-pass standard (like DoD 3-pass) is used and verified. |
| Purging | Advanced sanitization using degaussing (powerful magnets) or cryptographic erasure (destroying the encryption key). | Magnetic media (HDDs, tapes) needing high security or when wiping isn't feasible. Makes HDDs unusable. | Better: Offers a higher level of assurance; degaussing is irreversible. |
| Destroying (Shredding) | Physical destruction of the storage media by shredding, pulverizing, or disintegration. | End-of-life, damaged, or SSD drives. The ultimate solution for the most sensitive data. | Best: The only 100% foolproof method; data is physically impossible to recover. |
Choosing the right tool for the job is where you balance compliance with common sense. Making the wrong call can either leave your facility exposed or have you spending money to shred assets that still have plenty of value.
Matching the Method to the Mission
Let's dig into when and why you'd use each of these approaches.
Software Wiping for Reusable Assets
When you want to reuse, repurpose, or resell a device, software-based wiping is your go-to. Using specialized software to perform a multi-pass overwrite, like the industry-trusted DoD 5220.22-M 3-pass standard, effectively buries the original ePHI under layers of gibberish.
This is the perfect approach for:
- Computers and laptops being passed to another department.
- Servers with valuable hardware you want to put back into service.
- Functional medical devices with hard drives that can be remarketed.
Wiping lets you recover value from retired equipment by keeping the physical asset intact. To see how this works in detail, you can explore our in-depth guide to secure data destruction techniques.
Purging for Enhanced Security
Purging methods take security up a notch. A degausser, for example, unleashes a powerful magnetic field that instantly scrambles the data on hard disk drives (HDDs) and old backup tapes. It’s incredibly fast, but it’s a one-way street—the process also renders the hard drive totally useless.
Another powerful purging technique is cryptographic erasure. Here, the data is encrypted, and then the digital key used to unlock it is destroyed. The data is still there, but it's permanently locked in an unreadable state with no key to ever open it again.
It’s always worth remembering what’s possible with modern hard drive data recovery, even from damaged media. Knowing what the experts can do really underscores why you need a method that makes data truly and permanently gone.
Physical Destruction for Ultimate Security
When there’s zero room for error, physical destruction is the only answer. This is for devices holding highly sensitive ePHI, or for storage media that’s old, broken, or can't be reliably wiped (like most Solid-State Drives, or SSDs). The process is exactly what it sounds like—we feed the devices into industrial shredders that grind them into tiny, useless fragments.
Physical shredding is the non-negotiable method for:
- Retired servers that once held massive patient databases.
- Damaged or failed hard drives that can’t even spin up to be wiped.
- Old backup tapes, CDs, and other legacy media collecting dust.
- Any device where the risk of a breach is simply too high to consider anything else.
The stakes have never been higher. With the average healthcare data breach now costing an eye-watering $10.93 million and impacting 18% of teaching hospitals, regulators are focusing more on secure disposal. In fact, by 2026, 70% of facilities that adopt integrated, HIPAA-focused e-waste programs are expected to see a sharp drop in vendor complexity and audit stress. This is exactly why partnering with a certified expert for secure, documented destruction is no longer a "nice-to-have"—it's an absolute necessity.
How to Select a Compliant Disposal Partner for Local or Nationwide Service
Picking a partner to handle your medical equipment disposal is a huge decision. You're not just hiring someone to haul away old machines; you're trusting them with your legal compliance, your patients' privacy, and your organization's reputation. Whether you need services in a single city like Dallas or across multiple states, the vetting process is the same.
The right HIPAA-compliant medical equipment disposal services should operate like an extension of your own security team. They need an ironclad process that covers everything from pickup to final destruction.
So, how do you know who to trust? You need a checklist. Think of it as a pre-flight check before your assets ever leave the building. Asking the right questions upfront is the only way to avoid a compliance nightmare down the road. Any legitimate partner will welcome these questions and have clear answers ready.
The Non-Negotiable Starting Point
Start with one simple, direct question: "Can I see your Business Associate Agreement (BAA)?" A BAA is the legally binding contract that makes your vendor just as responsible for protecting patient data as you are.
If a company hesitates, doesn't have a BAA, or seems confused by the question, walk away immediately. That’s a massive red flag. A signed BAA is the absolute bedrock of any compliant partnership, no exceptions.
Next, you have to verify their certifications. These aren't just logos to make a website look good; they are proof that an independent auditor has confirmed their processes meet strict industry standards for security and environmental protection.
Insist on seeing these two:
- NAID AAA Certification: This is the gold standard for secure data destruction. It means the vendor follows audited, verified procedures for wiping, shredding, and handling all sensitive media.
- R2v3 or e-Stewards Certification: These certifications guarantee that all electronics are recycled ethically and responsibly, keeping hazardous e-waste out of landfills.
A vendor holding both certifications shows a serious commitment to doing things the right way, protecting both your data and the environment.
From Pickup to Proof
A compliant process is a documented one. Your partner absolutely must provide a clear, auditable paper trail that tracks your equipment from the second it leaves your dock to its final destruction. We call this the chain of custody.
Think of the chain of custody like a documented evidence trail in a legal case. It details who handled the assets, where they were transported, and how they were secured at every step, leaving no gaps for data to be compromised.
At the end of this process, you should receive the single most important document: a Certificate of Destruction. This serialized certificate is your official legal proof of compliance. It needs to list what was destroyed, when, and how, effectively closing the loop on your HIPAA obligations.
This decision tree shows the basic logic a compliant vendor follows to choose the right destruction method for each asset.
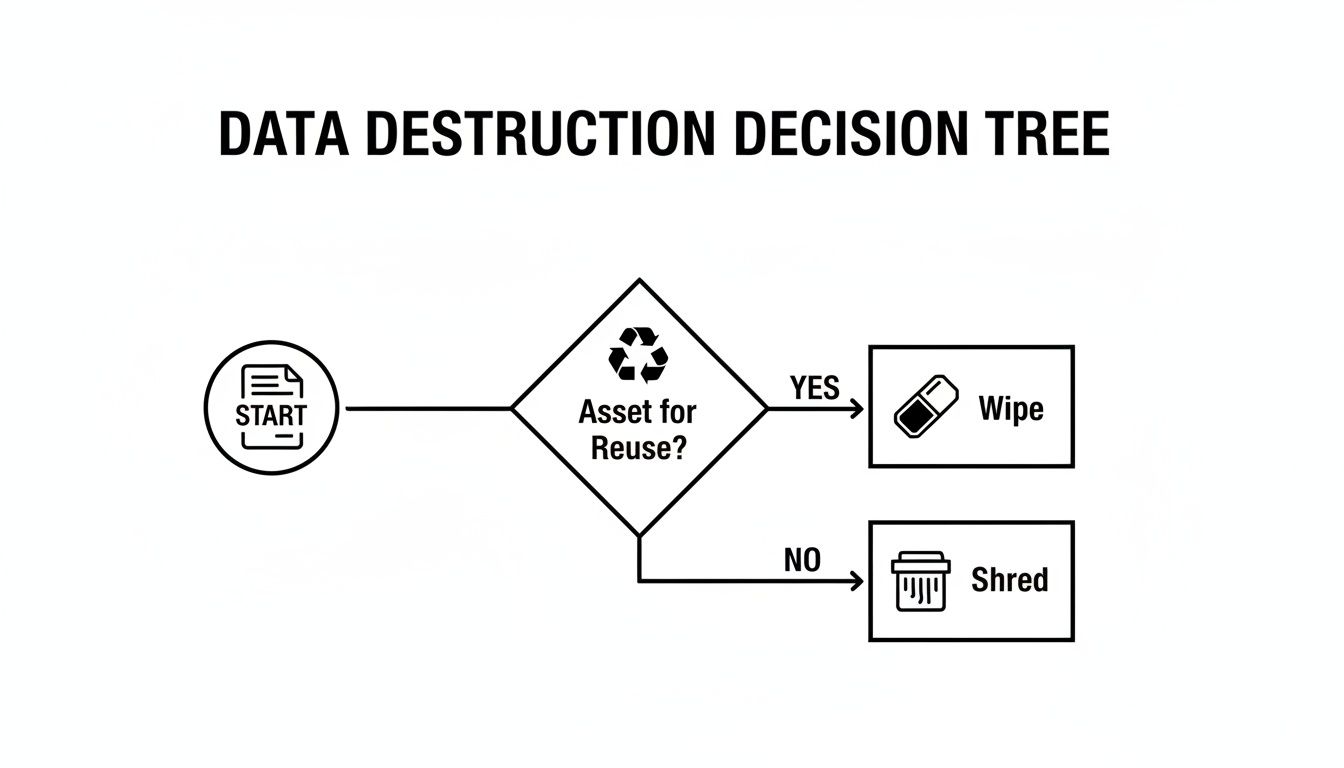
As you can see, the first question is always about reuse. If an asset can be remarketed, secure data wiping is the way to go. If not, physical shredding is the only way to guarantee total data elimination.
Evaluating Logistical Capability
Finally, a great partner needs the real-world muscle and resources to handle your specific project, whether it's a small local pickup or a nationwide rollout. This is especially true for large-scale decommissioning, which takes serious planning and coordination. You can find more on that in our guide to medical equipment decommissioning for healthcare facilities.
Ask them about their on-site services. Can they de-install large, complex systems? Do they operate their own fleet of secure, GPS-tracked trucks? A partner that handles the entire process in-house—de-installation, packing, logistics, and destruction—offers a much tighter, more secure process with fewer third parties and less risk, whether you're in one city or a hundred.
Ensuring a Secure Chain of Custody and Certified Recycling
Sure, you’ve wiped the hard drives. But what happens to your old medical equipment on the journey from your facility to the shredder? Without a rock-solid, documented security process from start to finish, you’re still exposed to major risks. This is why a chain of custody is one of the most important parts of any compliant disposal plan.
Think of it as a detailed evidence trail for your retired assets. A secure chain of custody meticulously tracks every single piece of equipment from the moment our team picks it up. It answers the big questions: Who took it? When was it transported? Where is it now? And how was it secured every step of the way?

Why a Documented Trail Is Non-Negotiable
Any undocumented gap in that chain is a serious security hole. For healthcare providers—from a local Chicago practice to a nationwide hospital system—a solid chain of custody is your proof that you never lost control of sensitive assets. A professional HIPAA-compliant medical equipment disposal service provides this documentation as a standard part of their process, not an afterthought.
This entire process wraps up with your official, legal proof of compliance, which is usually a Certificate of Destruction. To see exactly what this critical document looks like, check out our guide on creating a Certificate of Destruction template.
More Than Security: Your Environmental Duty
Protecting ePHI is priority number one, but your responsibility doesn’t stop there. Old medical equipment is a huge contributor to electronic waste (e-waste), and it’s often packed with hazardous materials like mercury, lead, and cadmium. Just dumping these devices in a landfill isn’t just bad for the environment; it can also land you with steep fines and damage your organization’s reputation.
Partnering with a certified electronics recycler is a crucial part of a modern disposal strategy. It shows a real commitment to corporate sustainability and protects your brand from the bad press that comes with improper e-waste handling.
This double focus on both security and sustainability is what separates the pros from the amateurs. An ideal partner holds certifications for both, making sure your organization is buttoned up on all fronts.
This is becoming a bigger deal every day. The U.S. healthcare waste management market is projected to hit USD 35.36 billion by 2035, and a huge driver of that growth is compliant equipment disposal. The offsite treatment segment already holds a 68.93% market share because more and more hospitals are outsourcing to certified vendors for solutions that are cost-effective and can scale with their needs.
What to Look for in a Recycling Partner
When you’re checking out a vendor’s environmental practices, you need to see specific, verifiable credentials. Certifications like R2v3 (Responsible Recycling) or e-Stewards are the gold standard in our industry.
These certifications are your guarantee that the vendor:
- Follows Strict Environmental Standards: They are regularly audited to prove they manage hazardous materials safely and ethically.
- Prioritizes Reuse and Recovery: Certified recyclers work to salvage any usable components before breaking things down to raw materials.
- Maintains a Secure Downstream: They track all materials to their final destination, preventing them from being illegally exported or dumped in a landfill.
By choosing a partner with these credentials, you can be confident your old equipment is handled in a way that protects both your sensitive data and the planet. This complete, end-to-end approach is the mark of a truly professional and compliant service.
Of course. Here is the rewritten section, adopting the expert, human-written style from the provided examples.
Common Questions About Medical Equipment Disposal
When it's time to retire old medical equipment, a lot of questions come up. We get it. Getting the details right is critical for compliance, so here are some straightforward answers to the questions we hear most often from healthcare facilities across the nation.
What Types of Medical Equipment Actually Contain ePHI?
You'd be surprised. It’s not just the obvious items like EHR servers, office computers, or tablets. The list of equipment that stores electronic Protected Health Information (ePHI) is longer than most people think.
Many diagnostic machines—MRI, CT scanners, and ultrasound devices—all have internal hard drives that hold onto patient images and data. Even smaller, seemingly simple devices like patient monitors, infusion pumps, and digital thermometers can retain sensitive information. Don't forget the standard office gear in a healthcare setting, either. Printers, scanners, and fax machines often cache copies of every single document, creating a huge and often overlooked security risk. A professional HIPAA-compliant medical equipment disposal service knows to check every single asset for hidden data.
Is Deleting Files or Formatting a Hard Drive Enough for HIPAA?
No, not even close. Hitting "delete" or running a standard format on a hard drive is one of the biggest compliance mistakes you can make. These actions only remove the path to the data, leaving it completely recoverable with basic software. It's a method that falls dangerously short of HIPAA's requirements.
HIPAA is crystal clear: ePHI must be rendered "unreadable and unrecoverable." This isn't a suggestion; it's a mandate that requires professional data destruction.
To truly meet this standard, you need proven methods. This could mean a multi-pass data wipe (like the DoD 5220.22-M standard) that overwrites the information again and again. For 100% certainty, nothing beats physical destruction like shredding, which makes it impossible for anyone to recover the data.
Do These Rigorous Disposal Rules Apply to Small Clinics?
Yes. HIPAA rules apply equally to all "Covered Entities" and their "Business Associates," no matter how big or small they are. A local dental practice in Denver, a small specialty lab in Atlanta, or a solo practitioner has the exact same legal duty to protect patient data as a major hospital network.
For a smaller practice, a data breach can be even more catastrophic. The fines are massive, and the damage to your reputation in the local community can be impossible to repair. Partnering with a certified disposal vendor gives small clinics access to the same high-level security and compliance that large organizations rely on, but without the cost of managing it all in-house.
What Is a Certificate of Destruction and Why Is It So Important?
A Certificate of Destruction is the official legal document that proves you did your job correctly. Issued by your disposal partner, it's your paper trail for compliance.
This document meticulously records what was destroyed, when it was destroyed, the exact method used (like shredding or wiping), and lists the unique serial numbers of the assets. If you're ever faced with a HIPAA audit, this certificate is your number one piece of evidence. It formally closes the chain of custody and transfers liability from you to your vendor.
For healthcare facilities, labs, and universities in the Atlanta area and across the United States looking for a partner they can trust, Scientific Equipment Disposal offers a complete, on-site solution. We manage everything from de-installation and secure logistics to certified data destruction and responsible recycling, making sure your organization stays compliant. Learn more about our secure and sustainable nationwide services at https://www.scientificequipmentdisposal.com.